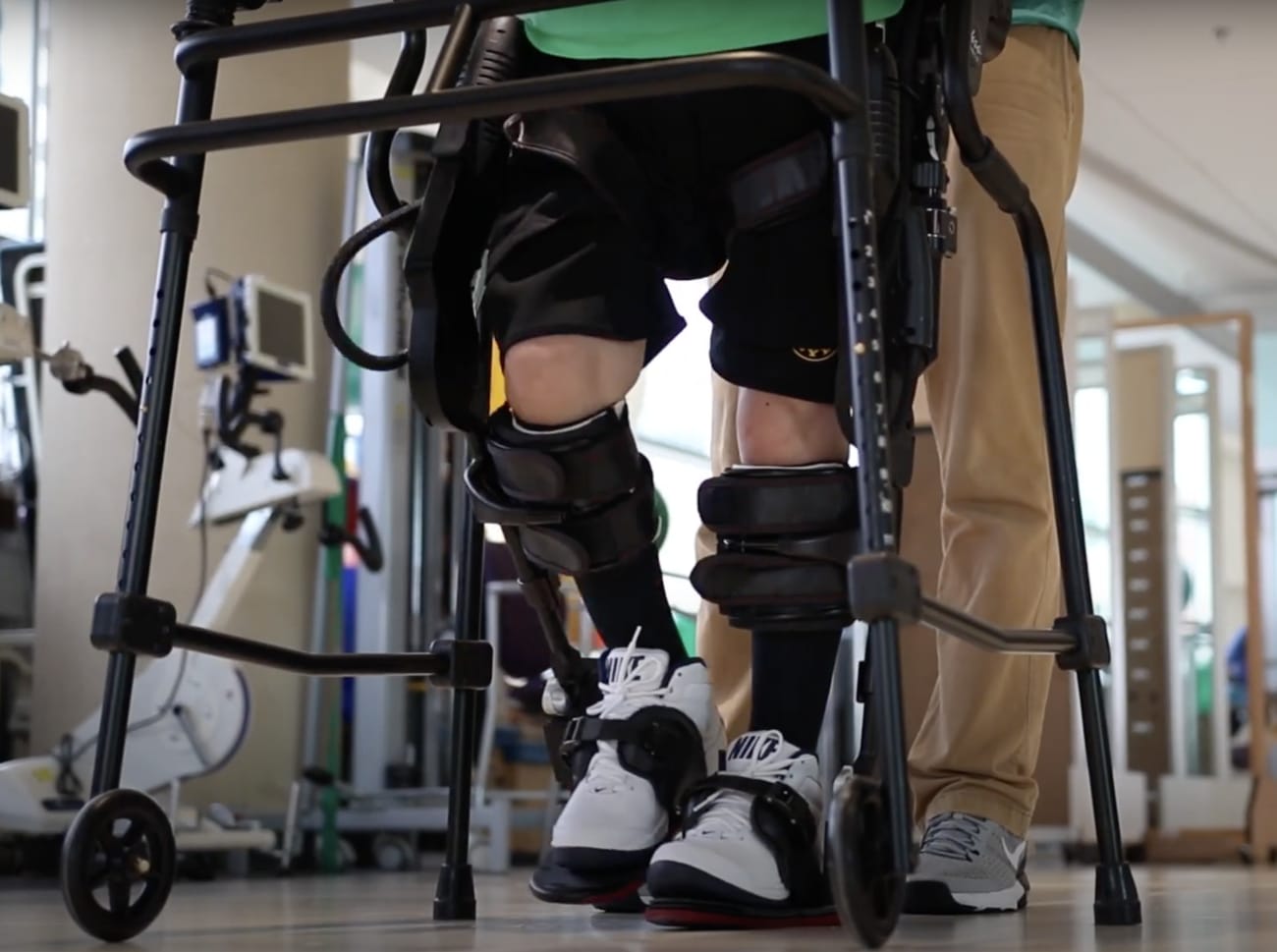
For patients with spinal cord injury and spinal cord disease-related paralysis, the International Center for Spinal Cord Injury offers individualized care and therapies with the aim of putting patients on a path to independence and better day-to-day neurologic function.
The center is a collaboration between the Johns Hopkins Department of Physical Medicine and Rehabilitation and Kennedy Krieger Institute. Its physicians and clinicians treat patients of all ages through specialized programs and advanced technology.
The center provides a rare combination of services: These include activity-based restorative therapies (ABRT) that use vetted neuroplastic principles of functional and neurologic restoration; adaptive sports; aquatic therapy; bone health; diaphragmatic and phrenic nerve pacing; nerve and tendon transfers; peer mentoring; a seating clinic; and spasticity management.
“We take care of the patient from top to bottom,” says Clinical Director Cristina Sadowsky. “Because we’ve been doing this for 20 years, we know how to mitigate the consequences of paralysis and optimize function.”
The center has one of the few adaptive sailing training facilities in the country, which allows individuals with various degrees of spinal cord injury and paralysis to learn how to sail in a virtual environment. Patients use hand-operated joysticks or “sip-and-puff” straws that control a boat by inhaling and exhaling. After training, they are able to navigate their own dinghies in the Chesapeake Bay. There are less than 20 such virtual trainers in the world.
Albert Recio, medical director of the aquatics medicine program at Kennedy Krieger Institute and one of the world’s foremost adaptive sailing experts, draws inspiration from Philip Craven, the second president of the International Paralympic Committee.
“The committee’s overarching philosophy is that sport is a human right, and every human, regardless of their ability or where they live, should have access to sports,” Recio says. “Hopefully we can, in our own small way, help eliminate those barriers in the sport of sailing.”
The center also hosts the International Virtual Reality Sailing Symposium, a virtual summit that brings together 10 centers from around the world to discuss research and clinical practice around adaptive sailing training.
The aquatic therapy program’s team is also able to work with complex patients in the therapeutic pools, including patients with colostomies, suprapubic indwelling catheters and tracheostomies. The program is the only one in the world to have a clinical aquatic therapy tract for patients with ventilators.
The International Center for Spinal Cord Injury uses ABRT, including functional electrical stimulation, massed practice (repetitive intensive practice of functional activities), weight-bearing exercise, locomotive training and gait training to prompt the nervous system to “remember” how to move. Two or more therapists work with each patient at a time in two- to five-hour sessions, and many patients recover some degree of sensation, movement and independence.
The center has 10 different kinds of equipment that allow for partial weight-supported walking. In September, it became the first center in the world to have a gait and balance training system that allows patients to walk in any direction while being supported.
The team of faculty and staff at the center includes four spinal cord injury specialists, a nurse practitioner and 60 physical and occupational therapists — one of the largest numbers of therapists who specialize in spinal cord injury and spinal cord disease-related paralysis in the nation. A psychologist and two social workers who specialize in mental health counseling, several rehabilitation technicians and aides, aquatic specialists, child life specialists, a nurse intake coordinator and a nurse case manager are also important parts of the group. The center additionally works with the Johns Hopkins Myelitis and Myelopathy Center, as well as surgeons and oncologists.
Because the center is a collaboration between Johns Hopkins and Kennedy Krieger Institute, patients have access to novel treatments via clinical research.
“We can implement whatever is the newest and best discovery that is transferable to clinical practice,” Sadowsky says. “We deliver lifelong, comprehensive medico-rehabilitative care. We do translational research, we do advanced rehabilitative techniques, and we do lifelong, chronic care, from birth to gracefully aging with paralysis.”
To refer a patient, call 888-923-9222.